Insertion of Syrinx Shunt
A syrinx is a fluid-filled cavity inside the spinal cord. It can be caused by a number of different things, including spinal injury, bleeding, infection and tumours. It can also be associated with congenital problems, such as Chiari malformation. As syrinxes enlarge, they can cause significant neurological symptoms, and may require treatment, such as by diverting the fluid away from the spinal cord into another part of the body where it is absorbed (most commonly the peritoneal cavity, in which case it is called a syringo-peritoneal shunt).
Indications
Not all syrinxes cause major symptoms or need treatment. However, they can cause significant pain, weakness, problems with feeling (such as sensing hot or cold, or sharp objects), and problems with balance or walking, especially if they get large enough. Other ways in which syrinxes might present include changes in posture or spinal alignment, leading to deformity.
Procedure
The operation is performed under general anaesthesia (i.e. with you fully asleep). You will be lying face down with your chest and hips supported on cushions. Your surgeon makes an incision in your back, usually over where the syrinx is the largest or closest to the surface of the spinal cord, where it is can be easily accessed. A small amount of bone covering the spinal canal is removed to access the dural sac (the ‘envelope’ that contains the spinal cord), which is then opened. A tiny incision is then made in the back of the spinal cord to access the syrinx. A thin silicone tube (i.e. the shunt) is then passed into the syrinx to let fluid drain. A separate incision is then made in the front of the abdomen, so that the other end of the tube can be passed into the peritoneal cavity. If for whatever reason the abdomen cannot be used, this other end of the shunt can also be inserted inside the pleural cavity, which houses the lungs. In other situations, a much shorter tube draining the syrinx into the so-called ‘subarachnoid’ space (i.e. all contained within the dural sac) might be used. Sometimes, a focal band ‘tethering’ the spinal cord may be identified, which needs to be cut in order to ‘free’ the spinal cord. After your surgeon has thoroughly irrigated your wound and is happy that there is no bleeding, the dura, soft tissue layers and skin are all closed with sutures.
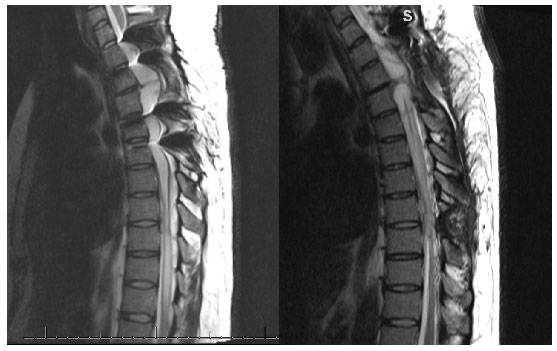
Figure. Before (left) and after (right) syringo-peritoneal shunt.
Risks or complications
Like other tubes or shunts inside the body, syrinx shunts can become blocked or infected, and may need to be removed or ‘revised’.
They may also drain too much fluid, or not enough.
Problems at the other end of the shunt include damage to the bowel. If the other end is inserted into the pleural cavity, large volumes of fluid can build up (termed pleural effusion), causing breathing difficulty.
Other surgical risks include wound infection, bleeding, leakage of spinal fluid (termed CSF), and damage to other nerves or spinal cord.
Anaesthetic and medical risks include heart or breathing issues, chest or urine infections, and blood clots in the legs (termed DVTs, which may travel to the lungs, causing PEs).
Postoperative instructions
Every patient’s recovery is different and may be influenced by how bad their symptoms were prior to surgery. In general, patients spend a few days in hospital after a syrinx shunt. The first day or so may be spent in bed lying down to give the dura the best chance of sealing (to prevent spinal fluid leak). Your surgeon will ensure that you have everything you need before you go home, including extra pain medications. Some patients might benefit from a short stint at rehabilitation before returning home. Most people should wait around 6 weeks before doing strenuous activity to give the body enough time to heal.
Adhering to the post-operative instructions provided by your surgeon is important to promote healing and reduce possible complications.




