Posterior Lumbar Fusion (PLF) and Decompression
Posterior Lumbar Fusion (PLF) and Decompression
In certain cases, a spinal fusion may be the recommended surgical procedure. The operation is used to join (fuse) together two or more vertebrae in the spine using a combination of screws, rods, and fusion devices with bone graft between the vertebrae.
There are a number of approaches to the lumbar spine: anterior, anterior-oblique, lateral, transforaminal and posterior (ie essentially from front, side or back). On occasions, your surgeon may use a combination of techniques to complete the surgical management of your condition.
The choice of approach is determined by the:
- Skill and preference of the surgeon
- Condition that is being treated
- Correction of deformity if present
- Degree of decompression required
- Safest approach for the individual patient.
Indication
Any fusion surgery should be considered carefully and cautiously. Performed for the incorrect or inappropriate reason can lead to poor patient outcomes. You must have that difficult conversation with your surgeon to understand the reason for surgery and what procedure is recommended.
Common conditions that are treated with PLF includes, but not limited to the following:
- Spondylolisthesis (slippage of vertebra)
- Scoliosis (significant curvature of spine)
- Recurrent disc herniation after multiple discectomy
- Foraminal disc herniations that require a significant facet joint resection
- Sagittal balance correction
- Mechanical back pain
Procedure
The surgery is performed general anaesthesia. You will lie on the operating table faced down and draped in a sterile fashion. One midline or two paramedian (parallel) skin incisions are performed. The muscles are disconnected from the bone, and the posterior portion of the vertebrae is removed to decompress the nerves and spinal sac. The facet joints are roughened to receive the bone graft. No fusion device (interbody cage) is used in the disc space. Screws and rods are inserted into the vertebrae from a posterior approach and the vertebrae is restored to the natural position and curvature. Your surgeon may use less invasive techniques and Navigation or Robotic Assisted technology during the procedure to minimise complications and improve outcomes.
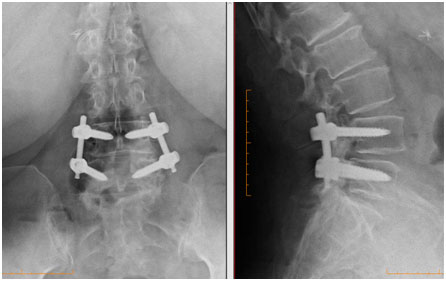
Risks or Complications
Includes but not limited to:
- Failure of bone healing
- Implant failure/migration
- Inaccurate positioning of implants
- Transient/Long term Nerve injury
- Transient/Long term Spinal cord injury
- Persistent nerve pain, numbness, tingling, burning, aching
- Persistent back pain/ache
- Infection
- Postoperative hematoma (bleeding)
- Spinal fluid leak (dural tear)
- Numbness above the incision site
- Slight reduction in motion of lumbar spine
Benefits
- Relief of nerve pain (leg pain)
- Relief of mechanical back pain
- Correction of deformity (better posture)
- Improved mobility




