Vertebral Compression Fractures
Vertebral compression fractures can occur as a result of trauma from a fall, a forceful jump, or a car accident or a tumour that spreads to the spine from elsewhere. Vertebral compression fractures usually are caused by osteoporosis, a condition that causes a thinning and softening of the bone. The thinning bones can cause tiny fractures during normal activities. In severe cases of osteoporosis, a simple movement like bending forward can cause spinal compression fracture resulting in kyphosis, a hump-like curvature of the spine.
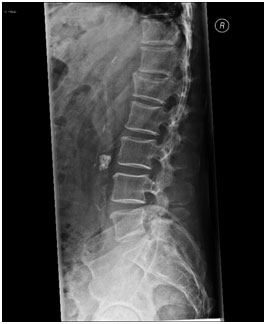
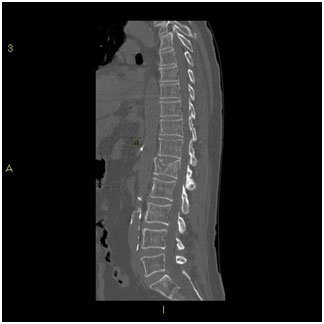
The most common symptom of vertebral compression fracture is severe pain in your back, which worsens on standing or walking and decreases when resting and lying down. You may also feel weakness and numbness in the affected areas, disability, and limited spinal mobility. You may also often notice a loss of overall height. Patients who sustain multiple compression fractures may have hunched back (kyphosis or "dowager’s hump"), gastrointestinal problems, hip pain, and shortness of breath. Rarely, you may suffer from neurological symptoms from nerve root or spinal cord compression.
Your doctor will carefully examine you based on the symptoms and medical history. Your doctor may also recommend other diagnostic tests such as:
· X-ray: A standing spinal X-ray (3 footX-ray or EOS) may be taken to determine the presence of a fracture and assess the kyphotic deformity
- CT scan: a CT scan may be performed to assess the extend of the fracture.
- MRI Scan: An MRI of spine may be performed to know if the fracture is old or new and to detect other soft tissue abnormalities
- Bone Scan and Spect CT: A nuclear bone scan may be used to help determine the presence or age of the fracture
- DEXA Scan: Dual Energy X-Ray Absorptiometry or DEXA scan, a test to measure bone mineral density, and is typically used to diagnose osteoporosis
Treatment
Non-Surgical
The treatment for vertebral compression fractures aims at reducing the pain and stabilizing and repairing the fracture. This is best achieved by medications, back braces, gentle ambulation and physical therapy.
Nonsteroidal anti-inflammatory drugs such as ibuprofen or naproxen may be prescribed to relieve bone, muscle and nerve pain. Your doctor may prescribe a back brace that supports the back and restricts movement.
Surgical
Surgery may be needed in patients who continue to have severe pain despite non-surgical treatment. Minimally invasive surgical procedures for treating vertebral compression fractures without breach of the posterior cortical bone where active healing is still present include:
Kyphoplasty : In this procedure a large needle is introduced into the spine with a balloon called a bone tamp and inflated until it expands to the desired height. The created space is then filled with or injected with orthopaedic cement called polymethylmethacrylate (PMMA). This procedure restores some height of the vertebrae and reduces some deformity.
Vertebroplasty : This technique involves inserting a cement material called polymethylmethacrylate (PMMA) into the bone of the collapsed vertebra with the needle and syringe under the guidance of X-ray. This technique is performed in order to stabilize the fracture and prevent further collapse.
Pedicle Screw Fixation and Fusion :If the kyphotic deformity is significant and pain is still an issue, minimally invasive pedicle screw fixation and facet resection and bone grafting may be necessary.
Prevention
The most effective way to prevent vertebral compression fractures is to prevent osteoporosis. A well-balanced diet, regular exercise program, calcium and vitamin D supplements, smoking cessation, estrogen hormone replacement for women and practicing good posture may help you to prevent osteoporosis.There are additional medications (eg Fosamax, Actonel, Forteo) that can also be used to improve bone density, and should be prescribed by an Endocrinologist that has a special interest in Metabolic Bone disease




